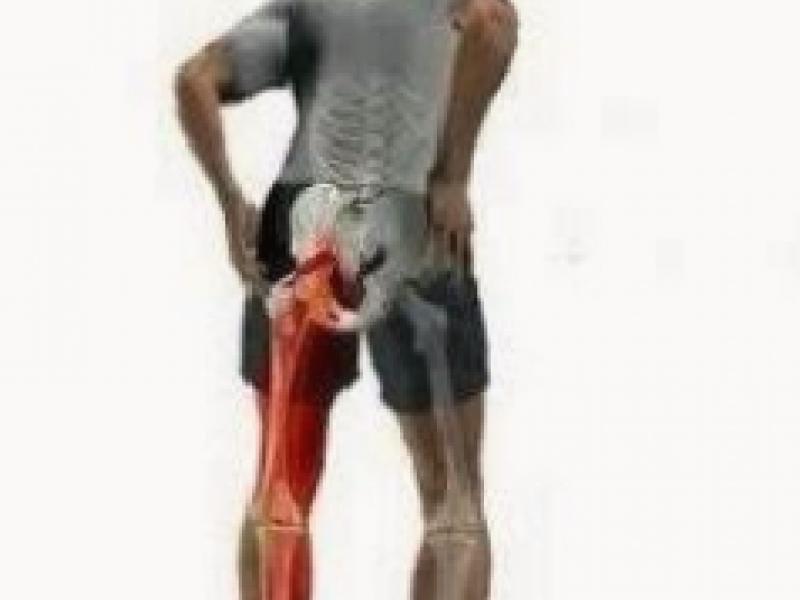
I- PAIN, DARKNESS AND LOSS OF FORCE
II- CHRONIC LOWER PAINIII-
III- ACUTE LOWER PAIN
A- Radiculopathy (Pain radiating from the waist to the leg)
B- Sciatica pain
C- Muscle spasms in the waist
D- Strain and sprain in the waist
A When we feel pain, it is a perception formed in our brain in response to signals carried throughout our body. These signals are the signals sent from the place where the pain originates. These signals are transmitted along the nerves and spinal cord to the brain, where they are perceived as pain.
Different types of pain
The origin of some pains is neuropathic while others are nociceptive. This is important to know because the treatment for each type of pain is different. Neuropathic pain is caused by damage to nerve tissue. These pains feel like burning or stabbing. An example of this type of pain is pain caused by nerve compression. Nociceptive pain, on the other hand, is pain due to injuries outside the nervous system. These pains are blunt pains. Examples of these pains are arthritis pains. Some patients may experience both of these pains.
Chronic and acute low back pain
Chronic low back pain is generally defined as deep, aching, blunt or burning pain that goes down to the lower back or leg. Patients may feel numbness, tingling or burning in their legs. Patients with chronic low back pain can hardly or cannot do their daily activities. Chronic low back pain tends to last very long and does not respond to standard treatments. This type of pain may be due to a long-standing injury, or it may be due to an ongoing illness.
Acute low back pain is usually described as very sharp pain or blunt pain. It is usually felt in the form of deep pain in the lower back and may be more severe in one area. Acute pain may be intermittent, but is usually continuous and can vary in severity.
Sometimes, acute low back pain may be due to injury or trauma. But often there is no known cause. Acute low back pain, even if severe, improves or passes within 6-8 weeks.
If acute low back pain is severe and spreads to the leg, it may be due to herniated disc.
Half of all patients with low back pain have acute pain due to trauma. Treatment of acute low back pain is usually short-term and successful. With physical therapy, follow-up and preventive measures, these patients regain all their functions within a few weeks. Patients with acute pain more than three times in a year or long-lasting attacks of low back pain that significantly affect their functional activities tend to develop chronic pain.
Mechanical low back pain
It is a type of acute pain. It increases with movement and worsens with coughing. This type of pain is usually relieved by rest. Mechanical pain is the pain seen in herniated discs and stress fractures. In these patients, bending forward usually causes pain. In addition, posture, coughing, stretching and movement affect spinal pain.
Drowsiness
Drowsiness occurs when nerve impulses are not transported properly from the skin to the brain. Patients with low back problems may feel numbness in their legs or feet. This indicates any nerve damage in the peripheral nervous system or the central nervous system.
The most common spinal (spinal) causes of drowsiness;
Radiculopathy: Nerve compressed due to herniated disc.
Stenosis (stenosis): Narrowing of the spinal canal.
Multiple sclerosis
Stroke
The most common cerebral (brain) causes of drowsiness;
Stroke
Seizure
Congenital anomalies
Concussion
LOSS OF FORCE
Weakness It occurs when impulses cannot be transmitted from the brain to the muscles properly. If there is a problem in the muscle itself, weakness can also be seen. If the muscle weakness is not due to diabetes or a similar systemic problem, the weakness may be due to a nerve or muscle problem.
The person’s general posture, gait, step size, and the degree and amount of swinging his arms while walking affect many muscles in the lower back. A minor injury that does not cause an obvious complaint causes the person to compensate for this injury in different ways while walking. Small and large adjustments that the person makes in his daily activities to compensate for this injury can sometimes cause sequential effects up to low back pain.
Causes of muscle weakness;
Myopathy
Myopathy is a systemic condition that affects the muscles, usually the muscles of the whole body. There are many types of myopathy, some of which are caused by; Diabetes, infections and other endocrine disorders resulting from autoimmune diseases are toxic and hereditary causes. Most myopathies first appear in the muscles near the trunk, upper extremities (arms), pectoral muscle (shoulder muscle), and thigh muscles.
People with myopathy may have difficulty climbing stairs, their knees may bend involuntarily, and they may have difficulty performing routine daily activities.
The most common neurological causes of muscle weakness;
Stroke
Spinal cord injury
Injury or damage to peripheral nerves
Myopathy
Osteoporosis-osteoarthritis
II- CHRONIC LACK PAIN
If you have pain for more than 6 months despite medical and/or surgical treatments, you have chronic pain. Chronic pain can be caused by a previous and healing injury or by an ongoing condition such as low back and/or leg pain, cancer pain, and neuropathic pain.
It is estimated that 15-33% of the population or 70 million people in the USA have chronic pain. The number of people who are unable to work and/or need care due to chronic pain is higher than cancer and heart diseases. Medical expenses caused by chronic pain are more than the sum of these two diseases.
Causes and treatment of chronic pain
Pain is a process. Receptors in our skin and other tissues send signals to our spinal cord via nerves. These signals are then transmitted to the brain. The place where the sense of pain is perceived is not the place where the pain is, but our brain. In other words, if the signals are prevented from reaching our brain, we do not feel pain. It is possible to relieve the pain of many people with drugs and other methods. However, sometimes it is not possible to relieve the pain or it is not possible to use this method due to the side effects of the pain-relieving method. Sometimes, the patient may continue to have pain due to the following reasons;
Some patients cannot tell about their pain because they think they will be perceived as a bad patient when they say they have pain.
On the other hand, some patients do not use painkillers because they think that they will become addicted when they use drugs continuously because of their pain. However, dependence on drugs is rare when used appropriately.
Some patients do not talk about their pain or seek appropriate treatment because they perceive talking about pain as a weakness.
It should be noted that today there are many new methods for the treatment of pain. If you have persistent pain, consult your doctor.
Chronic low back and leg pain is defined as pain felt in the low back and/or leg that may result from spinal diseases such as arachnoiditis, degenerative disc disease, epidural fibrosis, failed back surgery syndrome, herniated disc, osteoporosis (bone loss) and stenosis. . The pain is usually in the lower back, but may radiate to the thigh, calf, or foot. The affected area may be tender or painful to the touch and the pain may increase with movement. This type of pain can be like a stabbing pain, a burning sensation or a blunt muscle pain
Cancer pain
Cancer pains are generally divided into two groups:
Nociceptive pain: Nociceptive pain in tissue occurs due to damage. These pains are usually described as sharp, aching, or throbbing. These pains are often seen as a result of the tumor or cancer cells growing too large and filling the surrounding areas of the cancerous area. These pains can also be caused by the spread of cancer to the bones, muscles or joints, or by blockage of organs or blood vessels.
Neuropathic pain: Pain that occurs when nerves are damaged. It can be seen due to a tumor pressing on a nerve or nerves. This pain is often described as burning, may be accompanied by numbness.
Painful neuropathies
Painful neuropathies are a general group of neurological diseases that cause severe chronic pain as a result of nerve damage. Painful neuropathies can be caused by malnutrition, alcoholism, toxins, infections, or autoimmune causes, or due to diseases such as kidney failure or cancer. However, the cause of neuropathy cannot be determined in 1/3 of the cases.
Although there are many causes of painful neuropathy, the complaints of pain, burning, weakness and numbness are common in all of them. These symptoms usually occur in the hand or foot. Treatment is directed at the underlying cause, if known. Pain is usually treated with oral medications. However, some drugs that reduce nerve sensitivity, commonly known as epilepsy drugs, can be used to relieve pain in neuropathic pain.
III- ACUTE LOWER PAIN
A- Radiculopathy (Pain spreading from waist to leg)
Doctors use the term radiculopathy as pain in your arm or leg, numbness, Used to describe tingling and tingling. Nerve roots are branches of the spinal cord and carry nerve impulses throughout the body at all spinal cord levels. Radiculopathy is usually the result of a hernia compressing the nerve. However, it can also be seen as a result of degenerative changes that cause irritation and inflammation in the nerve root. A patient with radiculopathy may experience numbness and weakness in different regions, depending on the pinched nerve root in the arm or leg. Nerve roots at one or more levels; Since it may be under unilateral or bilateral pressure, the signs and symptoms may vary accordingly. Since each nerve root spreads in a certain part of the body, it may be possible to detect the compressed nerve root or roots with the findings in the examination.
Symptoms
The most common manifestation of lumbar radiculopathy is sciatica. This is a pain that radiates from your lower back to your hips and legs. Sensory symptoms are more common than signs of loss of strength. Loss of strength indicates more severe nerve compression. The quality and type of pain can be very variable. Radiculopathy may produce hypersensitivity or numbness to touch in the area of the nerve under compression. Symptoms such as numbness, tingling and tingling, especially leg weakness along with low back pain indicate that your problem is serious and you should definitely see a doctor.
Diagnosis
Radiculopathy has many causes. The first thing to do in order to determine the condition causing radiculopathy is a systemic examination to be performed with special attention to the waist and leg regions. Your doctor will check your lower back for flexibility, range of motion, and any signs of compression of the nerves. For this purpose, your muscle strength, sense and reflexes will be checked.
Patients who apply to a doctor with low back pain are usually first taken with direct x-rays. Magnetic Resonance Imaging (MRI) or Computed Tomography (CT) can be taken if further examination is required. Since MRI is very useful in the evaluation of soft tissues such as nerves and discs, it is a very useful examination in determining where the nerve root is compressed. CT, on the other hand, is a very useful examination, especially in the evaluation of bone structures. For this reason, it is very useful in the evaluation of the bone structures surrounding the spinal cord and nerve roots.
CT or MRI is usually not required unless a condition that may require surgery is detected. MRI is usually taken in cases where the diagnosis cannot be fully confirmed, medical treatments do not relieve symptoms, and surgical planning is required.
Treatment
After your diagnosis is made, your doctor will discuss treatment options with you. In patients without nerve compression causing muscle weakness, treatment usually includes the use of non-steroidal anti-inflammatory (NSAI) medication, rest, and physical therapy. A soft waist or neck brace may be given for short periods of time to provide rest for the lower back or neck.
Surgery in patients with radiculopathy is performed in the early period in patients with nerve compression that has only caused muscle weakness. Because muscle weakness is much more serious than just pain, it indicates injury to the nerve. Therefore, the pressure on the nerve must be removed first.
B- Sciatica pain
Sciatica pain is the name given to pain that starts in the hip and thigh and radiates down the leg. This pain is often accompanied by low back pain. Low back pain may be more severe or less than leg pain. True sciatic pain occurs as a result of compression of one of the nerve roots involved in the formation of the sciatic nerve due to a herniated disc. This type of low back pain is less common than other low back pain causes and conditions. For example, sporting activities, recreational activities and heavy work can cause lower back and leg pain and are often mistakenly diagnosed as sciatica. It is important to distinguish between these two types of pain. While true sciatic pain is due to nerve compression, the second type of pain is seen as a result of strain and sprains in the musculoskeletal system.
Signs and Symptoms
The most common symptom of true low back pain is pain radiating to the back of the thigh, calf, and foot, which can be much more severe than the accompanying low back pain. Patients usually have moderate to severe pain that starts in the hip and goes down to the foot. It is important to know that true sciatic pain radiates below the knee. Patients often have low back pain that started a few days or weeks ago. Later, leg pains become more severe than low back pain, and sometimes even low back pain may disappear completely. However, in patients with prolonged sciatic pain, the pain may be localized to the back of the hip and leg.
Sciatic pain often does not involve a trauma or compulsive movement at the onset. Standing, sitting, lifting heavy, sneezing can increase the pain. Lying down is often the most controlled position.
Diagnosis and Treatment
A complete physical examination and medical history is the first thing to do in diagnosing sciatica. Nerve root stretching tests may then be performed to confirm the diagnosis of sciatica. For this purpose, the sciatic nerve can be tried to regress by raising your leg straight, or the body can be placed in certain positions to see if the pain recurs or increases.
In many patients, this pain goes away on its own, and patients who require medical attention are usually given short-term rest, restriction of movement, and non-steroidal anti-inflammatory (NSAI) drugs. A home program consisting of physical therapy, stretching and strengthening exercises is very beneficial for the patient to return to their daily activities as soon as possible. There are surgical options for patients who have very severe and unbearable pain or who have a herniated disc in their examinations. Patients with progressive neurological deficits and pain benefit more from surgery than patients with only pain without muscle weakness.
C- Muscle spasms in the lower back
Muscle spasm, which is one of the body’s natural and protective response mechanisms, is the involuntary and prolonged contraction of muscle fibers in response to injury or in response to inflammation in the muscle itself or in the nerve. Muscle spasms in the lower back can be a sign of damage or injury to underlying spinal structures such as the vertebrae, discs, and ligaments.
The symptom of muscle spasm is acute neck and low back pain accompanied by severe muscle tension in the neck or lower back, depending on the site of injury.
Muscle spasms can be caused by different reasons: Sudden or prolonged trauma to the spine or the muscles and tissues supporting the spine, or other types of mechanical disturbances that can cause compression or irritation on the spinal nerves.
How can muscle spasm be treated?
Home Treatment
In most cases, if there is no serious underlying medical problem or spinal condition, muscle spasms can resolve within a few days or weeks with conservative treatment. However, if you have the following complaints, you should immediately consult a doctor:
Urinary and/or bowel incontinence.
Muscle weakness in the legs or arms. Disruption of gait. Decreased walking distance.
Pain and/or numbness that descends into your legs or arms.
Pain that gets worse when you lie down or pain that keeps you up at night
Pain with fever, weight loss, or other signs of illness.
If neither of these are present, there are things you can do yourself to relax your sore muscles and reduce the inflammation that is causing the problem.
It is often thought that in such a situation, immediate bed rest is required. But this is not such a correct practice. It is better to continue normal daily activity at a slower pace and avoiding the movement that caused the injury. So you should avoid lying down for long periods of time.
In the first 72 hours of injury, cold application can be applied on the injured muscle for 20 minutes, many times during the day. Cold reduces inflammation and swelling, numbs tissue, and slows nerve impulses to the injured area. However, it is not correct to make cold application longer than 20 minutes. Because it can cause increased tension in the muscles and inflammation in the tissue.
After the first 72 hours, heat can be applied to reduce muscle tension and increase blood flow. Waiting 72 hours is for the initial swelling and inflammation to subside. Hot application should be done with wet heat, not dry heat, as there is a possibility of dehydration. In other words, instead of applying an object filled with hot water to the injured area, it is better to put a towel soaked in hot water, take a hot shower or enter the jacuzzi.
The use of non-steroidal anti-inflammatory drugs such as aspirin, ibuprofen, acetaminophen or naproxen sodium can reduce pain, swelling and stiffness.
Short-term use of a soft girdle or brace can help reduce muscle spasm by immobilizing inflamed tissues or spinal structures. However, this should be avoided as girdles and corsets weaken the muscles when used for a long time. Otherwise, later on, it will be easier to be injured due to muscle weakness.
If your complaints have not improved significantly after the first 72 hours, you should definitely consult your doctor. Because the underlying cause of your complaints may be a serious condition.
Massage therapy is a method of applying pressure or vibration to soft tissues of the body such as muscles, connective tissue, tendons, ligaments and joints. It can be applied to relax muscles, relieve pain, improve circulation and reduce tension.
During physical therapy, different treatments such as heat and cold application, ultrasound, hydrotherapy and massage are used together to reduce muscle pain and tension. In ultrasound application, low and high frequency waves are sent into the muscles to warm the muscles and increase blood circulation. Therapeutic and stretching exercises can be applied to restore muscle strength and maintain range of motion.
Preventing Re-injury
To prevent re-injury to your neck and lower back, it is important to establish and maintain the strength and flexibility of the muscles, tendons, and ligaments that support your spine. You can achieve this in the following ways;
You can regularly do sports such as cycling, swimming and walking that do not put excessive strain on your back and do not strain your joints. If you do not have the opportunity to do sports and exercise outside, you can use a treadmill or exercise bike at home.
Light stretching exercises can be done to provide and maintain flexibility. Stretching also helps regulate blood flow to the muscles.
D- Low back strain and sprain
After a hard working day, a sudden movement or injury, there is a strain or sprain in a sore back, muscles and ligaments. There is a load on the waist during bending, twisting and lifting heavy loads. This can result in injury, especially in people with weak lower back muscles.
When the muscles surrounding the spine are stretched too much, when they are under a very heavy load, when they are moved in a way that causes small tears in these muscles, there is usually a strain on the lower back. As a result of rupture of ligaments and muscles, microscopic hemorrhages into the muscle usually occur, causing swelling and painful spasm in the muscles. Frequently, injured muscles become sensitive to touch. Pain and spasm are the body’s way of telling you that a muscle is injured and should no longer be used. As a result, during this period of acute pain, one should avoid using the injured muscle, rest, apply cold or heat, and light massage to relieve spasm.
A forced back injury can take different forms; the muscles that support and move the spine may be injured; The ligaments that connect the vertebrae and form a strong capsule around the facet joints may be caused by a partially ruptured or slightly slipped disc. In each of these situations, the human body can usually heal on its own.
Low back strains and muscle spasms are very common, and unfortunately there is no treatment that will cure these types of injuries immediately. However, most low back strains can be successfully treated with non-steroidal anti-inflammatory drugs, short-term rest, and gradual return to normal activity. A physical therapy program consisting of stretching and strengthening exercises helps patients recover more quickly.
You should consult a doctor immediately if the following complaints develop when you have difficulty in your lower back:
If you cannot hold back your urine or bowel movements
Weakness in your leg muscles, deterioration in walking, gradual decrease in the distance you can walk
Pain and numbness that increases when coughing, sneezing and sitting, radiating down your leg
Pain that wakes you up at night or increases when you lie down
E- Trauma
From spinal trauma When mentioned, an injury to the bony structures, soft tissues and/or nerve structures of the spine is mentioned. What a neurosurgeon is most interested in in spinal trauma is whether there is an instability of the spine, the presence or possibility of a neurological injury.
The stability of the spine deteriorates when there are deteriorations in bone structures and ligaments. Instability in the spine may cause the spine to be unable to carry normal loads, permanent deformities, severe pain, and in some cases, serious nerve injuries. Frequently, instability develops as a result of fractures in the bony parts of the spine.
Fracture and dislocation occur together in trauma cases and can cause a highly unstable spine. The neurosurgeon tries to provide mechanical stability by intervening in the unstable area to prevent further neurological deficits and progressive deformities.
Post-traumatic injuries;
Fractures
Ligament injuries
Musculoskeletal injuries
a-Fractures ;
Compression fractures
The most common fractures in the lumbar region are compression fractures, which usually develop after a fall. These fractures can be detected by direct radiographs. Most compression fractures can be treated with rest, medication, and physical therapy.
Burst fractures
Burst fractures occur as a result of strong compressive loading that causes insufficiency in the anterior and middle column of the spine. In burst fractures, the length of the vertebrae is considerably reduced.
These fractures are unstable and require immediate intervention.
Flexion-compression fractures
Flexion-compression fractures are usually at the T1 and L1 levels. The degree of insufficiency of the anterior column depends on the severity of the compressive force. In these fractures, there is a slight decrease in vertebral height, but the middle and posterior column are intact. These fractures are considered stable.
Flexion-distraction fractures
These fractures are usually caused by seat belts in automobiles. In these fractures, failure develops in all three columns of the spine. Injury to the bone, ligaments, and disc can occur. These fractures are considered unstable and require immediate intervention.
Compression-torsion-translation fractures
While the effects of compression occur at the edges of the vertebral body, torsional and translational forces affect the vertebral body or disc and ligaments.
b- Ligament injuries;
When the body is in a weak state, the muscles cannot tolerate excessive stretching or there is tearing of the ligaments. In both cases, it causes strain and sprain in the waist. When this happens, the spasm immobilizes the muscles in the injured area to protect the ligaments and joints from further damage.
Ligament injuries occur after traumatic events and recovery may take 6-12 weeks depending on the severity of the injury. In the injury, the ligament may be strained, sprained, or torn. The treatment for each of these conditions is different.
The ligaments that control the lower back joints can be damaged by an accidental fall or slip. Lumbar sprains are caused by strain injury to the ligaments of the pelvis. The cause of a sprain in the waist is very similar to the cause of an ankle sprain, and the treatment and recovery process is similar. Applying firm support to the pelvic ligaments protects the ligaments from further strain as they repair and become strong again.
A patient with a low back sprain is more likely to be able to continue with his daily activities than a patient with a sprained ankle. The most important reason for this is that the ligaments in the ankle cannot be supported with a hard bandage. However, it should be noted that the danger of ligament damage in the waist is much greater than anywhere else in the body.
Bel ligament yaralanmalarının en sık sebepleri
Uzun bir süre ayakta kalmak zorunda kaldığımızda sıklıkla vücut ağırlığımızı bir bacağımızın üzerine bindiririz. Bunu yaptığımızda vücut ağılığımızın üçte ikisi pelvisimizin bir tarafındaki ligamentlere biner. Bu basit hareket omurganın şeklinin bozulmasına ve duruş bozukluğuna neden olur. Sonunda bu ligamentler ciddi bir bel yaralanmasındaki kadar zarar görebilir.
Kötü duruş ciddi ligament hasarına sebep olabilecek başka bir basit harekettir. Uzun süre sırada beklemek, bir partide ayakta durmak ve alışveriş yapmak yorucudur. Pek çok kişi böyle bir durumda fark etmeden, bu yorgunluğu telafi etmek için bir yana doğru eğilir. Bunu yaptığımızda tüm vücut ağırlığımız pelvis ve belimizdeki ligamentler çekmeye başlar. Bunu sürekli yapmak yıllar içerisinde zarar verir. Bu ligamentlerin sürekli gerilmesine ve gevşemesine neden olur ve sonunda bu ligamentler eklemlerinizi uygun şekilde kontrol edemez. Bu ayakta durmanın yarattığı basit zorlanmanın rahatsızlık, hatta ağrı oluşturmasına neden olabilir.
İş ortamında yaptığımız kaldırma, eğilme ve dönme hareketleri de ligamentleri sürekli ve tekrarlayan bir zorlanmaya maruz bırakabilir. Eğer ligamentler aşırı gerilir ise bel eklemleri uygun pozisyonda daha uzun süre tutulamaz ve bu ciddi bel burkulması ile sonuçlanabilir.
Egzersiz belimizdeki kasları güçlendirmek ve ligament yaralanmalarını önlemek için iyi bir yol olmasına rağmen, sportif aktiviteler ligament yaralanmalarının ve bel zorlanmalarının en sık sebebidir. Belimiz zorlanmaya karşı hassastır ve güçlenmek için egzersize ihtiyaç duyar, fakat, bu egzersizler eklemlerimiz için zararlı olabilir. Özellikle aşırı hareketler ve zorlamalar gerektiren sporlar zamanla hasar verebilir.
Kilo, belde ligament zorlanmasına neden olan bir diğer etkendir. Özellikle de karın bölgesindeki aşırı kilo zararlıdır ve anormal duruşa neden olur. Yağları yakan aerobik egzersizler, kas oluşturan kuvvet egzersizleri ve yoga gibi egzersizler kilonuzu kontrol etmeye yardımcı olur.