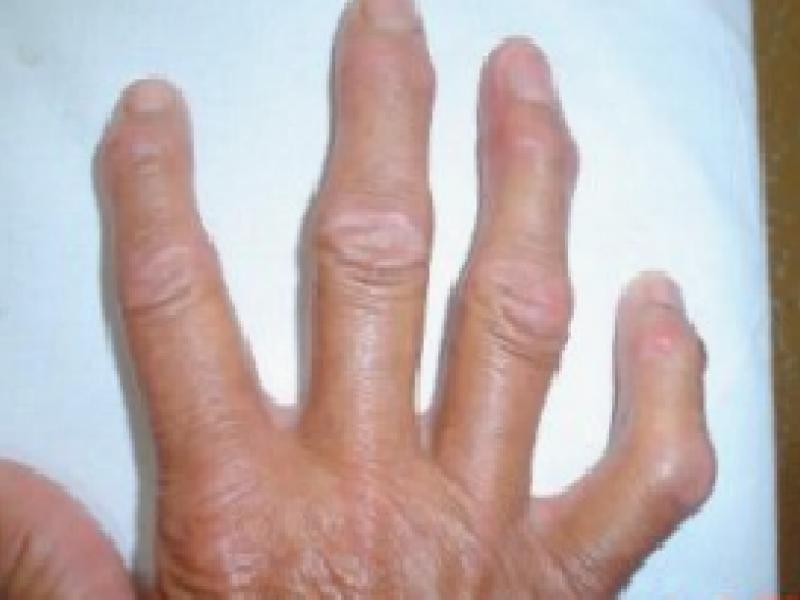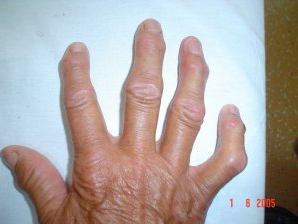
What is osteoarthritis?
Our bodies age as we age, and time changes our bodies without us even realizing it. Few people truly respect their health from their youth. Sometimes our life conditions are heavy and we work with body power, sometimes we force our body unnecessarily. The disease, which is known as calcification among the people and which we call osteoarthritis in the medical literature, is the disease of misused bodies.
One out of every 5 women and every 10 men over the age of 60 develops osteoarthritis. This disease comes to mind in our patients, who usually come with aging, especially in knee, hip, waist, back and hand pain. Difficulty in walking due to knee and hip pain, low back pain that increases with standing, pain at the root of the thumb and development of bone protrusions in the fingers are the most common complaints of our patients. Although prosthetic surgeries are the last treatment point in osteoarthritis today, the right treatments that can be applied to patients should be determined and preventive medicine should be performed until this treatment method is adopted.
The most important reason for the development of osteoarthritis is mechanical problems. Our joints are sensitive to overloads. Overloading, or the continued use of certain movements for a lifetime, causes the joints to begin to wear out. With age, the self-repair and regeneration properties of cartilage also decrease. Conditions causing calcification for today;
1. Increasing age; Over the age of 60, the risk of osteoarthritis increases more markedly each year.
2.Excess weight; The load that each body carries more than its ideal weight increases this risk even more. On the other hand, while this weight load is less on the hips, it is much more pronounced on the knee. I think one of the most important factors here is the way we walk. The wrong footing habits eventually expose the knee joint to a trauma with every step outside of its natural stance. Such traumas also cause the cartilage structure to become edematous over time. As this situation continues, a constant repair effort takes place in the knee cartilage, which triggers osteoarthritis in the future. If two women of the same weight who spent their life in the field and in a house without stairs are compared, it can be better understood the negative effects of uncontrolled stepping on the ground as a result of continuous work in the field. On the other hand, it should not be forgotten that osteoarthritis can develop in a thin person.
3.Being a woman; It is thought that the hormonal balance that changes with age and the lack of estrogen have an effect on the cartilage structure.
4. Joint injury traumas; What I mean here are blows to the string. Events such as jumping from height and falling should be understood.
5. One leg longer than the other 1 cm; A small and inexplicable leg difference will always have a traumatic effect on the short leg. Many years will pass without realizing such a small difference and the person will develop osteoarthritis.
6.Genetic characteristics; The truth of the matter is that 11 genes are thought to be associated with calcification. However, this effect was found to be extremely weak. Joints should be handled differently in terms of calcification. For example, the genetic predisposition for “erosive osteoarthritis”, which we will call damaged hand arthritis, is different and more pronounced than knee and hip. There is a correlation between the condition of my mother-aunt-aunt’s hands, which is especially true for women, and the possibility of the patient’s hand being similar. They can be listed as
. The most prominent among these factors are age and weight.
How do we know that the disease has developed?
It was believed for years that this disease was a non-inflammatory rheumatism. However, in the light of my belief and the latest data, it shows that the disease also includes a rheumatic reaction of its own. This difference in understanding brings osteoarthritis closer to the class of treatable diseases.
The first step in diagnosing this disease is to listen to the complaint thoroughly. We need to know which joint or joints have pain and at what times of the day these pains occur. In osteoarthritis;
Pain increases with movement.
Pain subsides when resting. You get up in the morning without pain and the pain increases during the day.
Stairs, folding one’s knees in prayer, sitting down meals and using the classical toilet especially increase knee pain.
Changes in the hip joint progress more slowly than in the knee.
Handiwork, dealing with cold water also increases hand pain
Pain increases especially in the lower back and knees when standing.
When diagnosing
A good conversation with the patient and then the examination is the first step
Simple movies of the complained area are seen
Specialists and now especially all rheumatology Ultrasonography used by clinics is also a helpful and simple test in diagnosis.
If necessary, advanced imaging tests are requested (MR or tomography)
Rarely, it is necessary to carefully distinguish it from other inflammatory rheumatism
Filming is our guide. Here, impaired joint structures, narrowing and damage are understood. If surgery is not considered in a patient over the age of 60, MRI is an extremely unnecessary examination.
My comments on treatment methods
Early diagnosis is the first and most important step in treatment. Because if treatment is not started early in osteoarthritis, effective treatment is very difficult after permanent changes occur.
The most effective treatment method is to remove the factor that forces the joint. This factor is weight loss, as the most common form of osteoarthritis is in the knee joint. It is also an important preventive medicine to make sports a part of life from the age of youth.
Lifestyle changes should be made. While making this plan, different suggestions are made according to which joint is affected. For example, someone with knee osteoarthritis avoids stairs, and someone with hand osteoarthritis avoids knitting or manual cleaning.
Surgery is a bit confusing. It is still not clear whether arthroscopic surgeries on the knee joint are beneficial or not, and scientific articles indicate that there are no convincing results in this regard. Corrective surgeries without prosthesis can only be successful in very special hands and in selected cases. There are serious fears for prosthetic surgery. At this point, the fact that our patients, who are often older, have additional diseases such as diabetes mellitus, prevents the physician from performing surgery. It is known that prostheses have a certain life span and if a prosthesis is to be placed, the patient is asked to come for surgery at an advanced age. However, no matter how old we are, we want to live a quality life and enjoy life. While it is possible to eliminate a knee pain that keeps us out of bed at night with an operation at the age of 50, asking the patient to do this surgery when he/she is old is to want the patient to live his/her life in a poor quality. At this point, I always try to ask myself this question and say what would I want if it were me. I think it would be wrong not to do surgery to an 80-year-old and lively person just because of his age.
To date, a painkiller-based treatment approach has always been adopted in the drug treatment of osteoarthritis. However, the possibility of keeping the joint in the correct position for someone who takes painkillers constantly will decrease. While there is increasing evidence that osteoarthritis is also a partial inflammatory rheumatic disease, the effort to use only painkillers to treat this disease is an inadequate treatment approach. However, there are no drugs that we can call the definitive solution in this regard, and different treatment methods are emerging based on the experience of physicians. It is controversial whether hyaluronic acid and glucosaminoglycan, which have been increasing recently and are described as cartilage enhancers, are really effective, and they can be beneficial in the right cases.
Intra-articular cortisone application can be tried 1-2 times in the knee. However, repeated injections will also increase the rate of damage to the knee cartilage.
Cartilage transplants, growth hormone inhibitors, stem cell treatments have not yet provided satisfactory results.
The main treatment method for osteoarthritis of the shoulder joint and spine is exercise.
Recently, the PRP treatment, which is called stem cell therapy among the people, but which has nothing to do with stem cells in the real sense, has become increasingly common. My personal opinion on this issue is that this method is ineffective and the results of the study do not mention a good result in this direction.
Let’s not forget that hand osteoarthritis should be evaluated differently.